Ever been told your swelling is "normal" or to "just give it time"? If you're dealing with swelling after surgery or chronic edema, you know it's anything but normal.
That stagnant fluid isn't just uncomfortable; it's actively changing your body in ways that can impact your long-term health and recovery. Let's dive into what's really happening and why getting expert help matters.
Your Body's Drainage System: The Lymphatic Network
Think of your lymphatic system as your body's internal plumbing, a sophisticated network designed to drain excess fluid, proteins, and waste from your tissues, returning them to your bloodstream.
When this system gets overwhelmed (like after surgery) or damaged (as in lymphedema), fluid starts to build up.
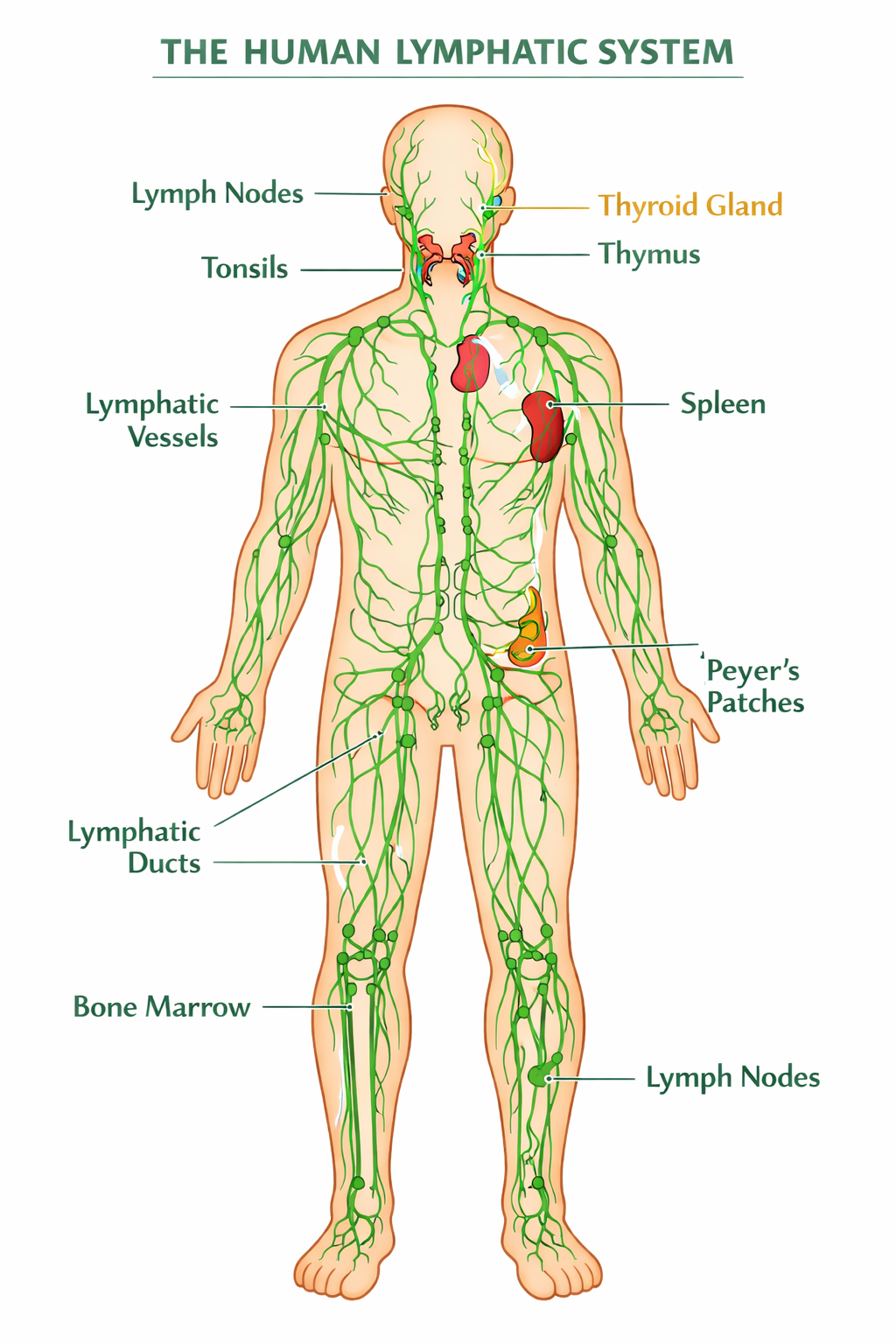
A simplified diagram of the human lymphatic system, showing its extensive network throughout the body.
This isn't just a cosmetic issue; it kicks off a chain reaction in your tissues.
The Inflammation Cycle and Tissue Changes
When protein-rich lymphatic fluid gets stuck, your body sees it as a problem and responds with inflammation. While inflammation is usually helpful, chronic, unresolved swelling turns this response into a problem, leading to significant tissue changes.
One of the biggest impacts is on your connective tissue, the framework supporting your muscles, skin, and organs. Persistent swelling can lead to fibrosis, essentially scar tissue forming. This makes your tissues stiffer, less flexible, and harder to treat over time.
Fibrosis Can Lead To:
- Reduced flexibility and range of motion
- Tight or "thick" feeling tissues
- Permanent changes if not addressed
A visual comparison illustrating normal skin versus swollen skin due to edema, highlighting the visible changes.
And here's a surprise for many: chronic swelling can also trigger abnormal fat tissue growth. Stagnant fluid activates signals that cause fat cells to grow larger and multiply. This isn't like regular weight gain; it requires specialized lymphatic care.
Your muscles also suffer. Swollen tissues compress everything, limiting blood flow and space for muscles to move properly. This is why limbs can feel "heavy" or "unwilling to move."
Finally, your circulation takes a hit. Increased pressure in swollen tissues reduces oxygen delivery and impairs waste removal, slowing down healing – crucial after surgery.
Skin Deep: Visible and Hidden Changes
Over time, chronic swelling leads to visible skin changes: thickening, texture alterations, and reduced elasticity. It also increases the risk of skin infections because your lymphatic system is vital for immune function.
These aren't just cosmetic; they're signs your tissues need help.
Why Acting Early Matters
The good news? Many of these changes can be prevented or minimized with proper care, especially when addressed early. The sooner you intervene, the better your outcomes because:
Early Intervention Benefits:
- Inflammation hasn't caused extensive tissue damage
- Fibrosis hasn't become established
- Your lymphatic vessels are more responsive to treatment
- You can prevent the progression from fluid-dominant to tissue-dominant changes
How Clinical Lymphatic Drainage Helps
Manual Lymphatic Drainage (MLD), performed by a certified therapist, is specifically designed to address these issues. While research varies, it's particularly beneficial for:
MLD Is Especially Beneficial For:
- Early Post-Surgical Care: Helps prevent progression to chronic lymphedema and supports healing
- Mild to Moderate Swelling: Can significantly reduce volume and manage symptoms before extensive tissue changes
- Symptom Relief: Reduces pain, improves comfort, and enhances quality of life
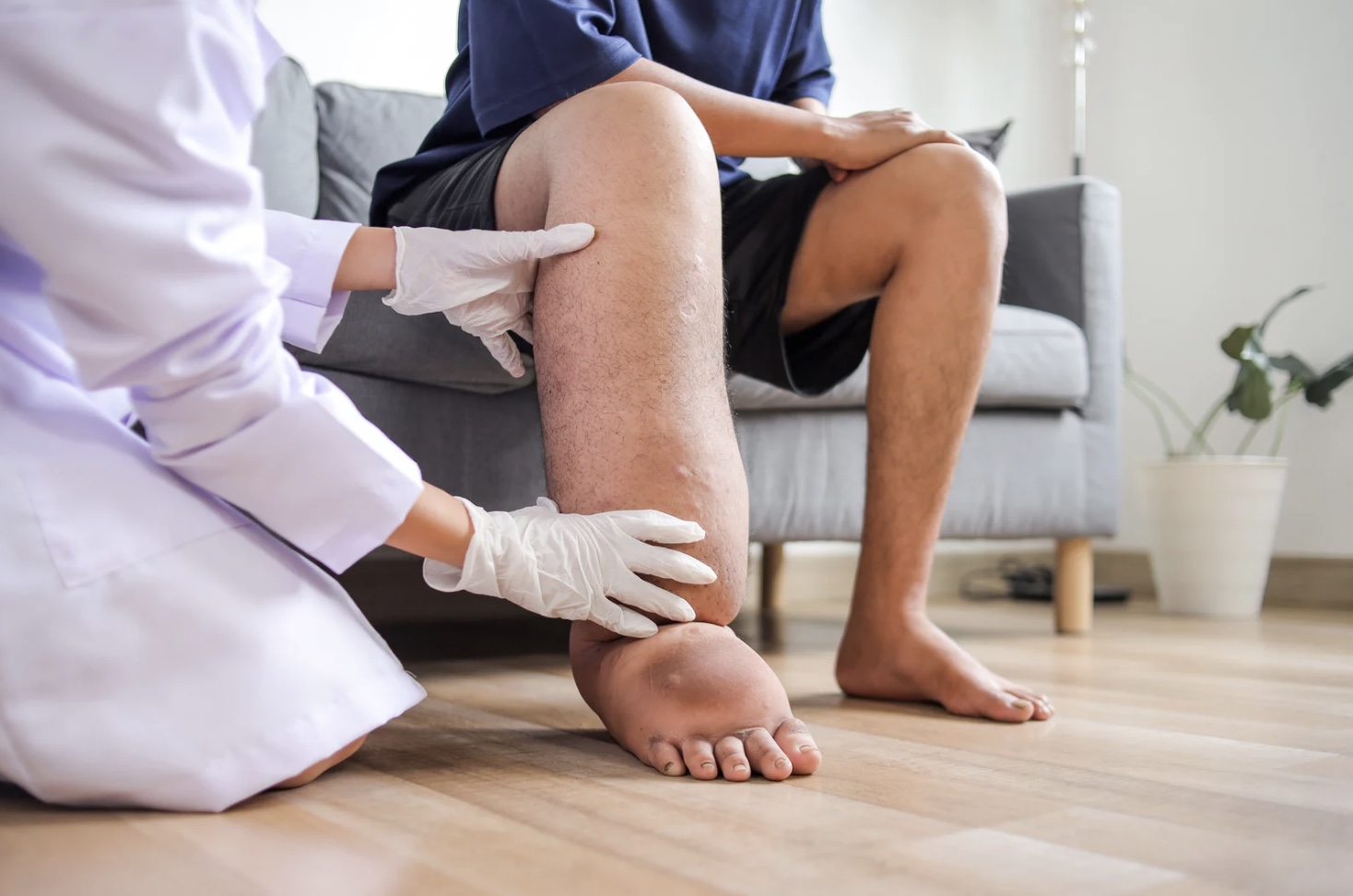
A certified therapist performing Manual Lymphatic Drainage (MLD) on a patient, demonstrating the gentle, specific techniques used.
MLD vs. Regular Massage: A Key Difference
It's crucial to understand that MLD is not a regular massage. While massage therapists offer wonderful benefits, MLD requires specialized training in:
MLD Requires Specialized Training In:
- Lymphatic anatomy and physiology
- Specific, very light pressure techniques
- Knowledge of drainage pathways and contraindications
- Certification through specialized lymphedema therapy programs
When dealing with lymphatic dysfunction, you need someone with specific expertise in this system.
When to Seek Expert Guidance
Consider consulting a Doctor of Physical Therapy who is also a Certified Lymphedema Therapist (DPT + CLT) if you're experiencing:
Signs You Should Seek Expert Help:
- Post-surgical swelling that isn't resolving
- Persistent swelling, heaviness, or discomfort
- Skin changes or reduced movement due to swelling
- A diagnosis of lipedema, lymphedema, or chronic venous insufficiency
A specialist with these dual credentials can accurately assess your condition, determine the best treatment, address both lymphatic and movement issues, and coordinate with your medical team.
Your Body Deserves Expert Care
The research is clear: stagnant lymphatic fluid and chronic edema are not minor issues. They cause real changes that impact your comfort, function, and quality of life. You don't have to accept "wait and see" as your only option.
Whether you're recovering from surgery or managing a chronic condition, specialized lymphatic care can make a meaningful difference in how your body heals and how you feel.
You deserve care from someone who truly understands the complexities of your lymphatic system.
Evidence-Based Care
This article is based on peer-reviewed research and evidence-based clinical guidelines. Specific citations are available upon request.
Ready to Take the Next Step?
As a performance specialist and musculoskeletal expert with over 20 years of experience, I provide expert guidance for post-surgical recovery and chronic swelling conditions.
Schedule a consultation to discuss how specialized lymphatic care can support your healing journey.
Schedule Your Consultation
